Bunions
What is it?
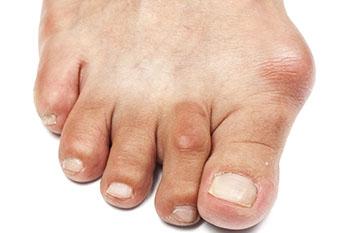
One of the more common conditions treated by a podiatric surgeon is a painful bunion. A bunion is a bony bump that forms on the joint at the base of your big toe. A painful bunion leads to restrictions of daily and recreational activities, difficulty in wearing shoes and overall decreased quality of life. A Bunion (hallux abducto valgus) occurs in both adults and adolescents. A bunion is not simply a bump, it is actually a dislocation of the 1st metatarsophalangeal joint. There is a medial deviation of the first metatarsal meaning the 1st metatarsal shifts away from the other long bones causing an increase in the angle between the 1st and 2nd metatarsal. At the same time this deviation leads to increased laterally directed pressure on the big toe. As a result of this, the constant pressure and friction will cause extra bone to form, leading to the bump that is seen on the side of the foot to become larger. The head of the 1st metatarsal becomes very prominent making it difficult to wear shoes due to pressure and becomes painful. As the deformity worsens as it does over time, the 1st metatarsal becomes unstable causing arthritis in the big toe joint, transfer stress to the 2nd metatarsal head as well as causing a hammertoe to the second digit due to the big toe pushing against the 2nd digit.
Why do I get a bunion?
Bunions are primarily genetic in nature, meaning that most people have a bunion because they inherited it from someone in their family. However there are numerous factors that have been proposed as contributors to the development of one. Inappropriate shoe wear, particularly high heels allow limited space for the forefoot pushing the big toe to the second toe as well as narrow shoes that might cause bunions or make them worse. Bunions can also develop as a result of an inherited structural defect such as an underlying flatfoot deformity or hypermobility of the medial aspect of the foot. This foot type can cause changes in the mechanics and muscle direction of the joint causing the shift of the 1st metatarsal because of the loose ligaments around it. Stress on the foot or inflammatory arthropathies, including rheumatoid arthritis and psoriatic arthritis are also predisposing factors.
What are bunion symptoms?
Bunions are not always painful, however when they are the location may mean different things. A patient may have a severe bunion with no pain, while another with a mild bunion can have significant pain. Shoes will typically aggravate bunions. The prime offenders are stiff leather shoes or shoes with a tapered toe box. Bunion pain is more common in women whose shoes have a pointed toe box. Pain medially may indicate bursal irritation, which is a fluid filled sac that provides cushion between bones and tendons that become inflamed from friction. Plantar pain may be indicative of sesamoid involvement because hallux valgus causes sesamoids to be in an abnormal position, therefore causing improper pressure. Pain on top of the joint implies arthritic involvement of the joint, which causes pain within the joint when walking. Patients can notice painful thickening of the skin (calluses) as well as swelling and redness along the medial bump. Occasionally, corns can develop between the 1st and 2nd toe from the pressure of the toes rubbing against each other. Other symptoms include numbness and a burning sensation along the prominence when rubbed in a shoe.
Diagnosis of a Bunion
Bunions are diagnosed by physical examination and x-rays. The overall alignment of the foot is visually inspected, including the arch height, lesser toe deformities, and any plantar calluses under the second or third metatarsal heads, which may indicate hypermobility of the medial column. Appropriate radiographic evaluation requires weightbearing views to determine the true extent of the deformity. Certain angular measurements are determined to aid in defining the type and severity of the deformity, which Dr. Fihman will explain to the patient in great detail.
Bunion Treatment
- Conservative Treatment
It is appropriate to treat a bunion non-surgically. Early treatment of bunions is centered on providing symptomatic relief. The patient must be educated about appropriate shoe wear, including wearing low-heeled shoes with a wide toe box and soft leather uppers to relieve pressure over the medial bunion. Various padding devices or cushions placed over the bunion may be helpful for mild bunion deformities as well as toe spacers between the big toe and 2nd toe. Strapping or splinting the big toe may partially reduce the deformity, but does not provide long-term benefit. Calluses can be shaved in the office periodically. Custom orthotics are recommended in alleviating symptoms in patients with flatfoot and associated pain along the metatarsals, as well as controlling abnormal pronation, which will reduce the deforming forces leading to bunions in the first place. These may help reduce pain in mild bunion deformities and slow the progression of the deformity. Corticosteroid injections can be useful in treating the inflamed bursa that is sometimes seen with bunions. When these conservative measures fail to provide adequate relief, surgical correction is indicated.
- Surgical Treatment
Surgical treatment is chosen for hallux valgus deformity when non-surgical measures have failed. Surgery may be the first method of treatment for a patient with a severe deformity with pain. The choice of surgical procedures is based on biomechanical and radiographic examination of the foot. The goals of surgery are a pain free joint, intermetatarsal angle less than 10 degrees, congruent joint, good range of motion, sesamoids in good position, a beautiful aesthetic result and to have the least chance of recurrence. There are a lot of myths about the recovery after bunion surgery. Most of our patients experience minimum to no pain after surgery. Based upon radiological and clinical assessment the surgeon must decide the right choice of procedure.
Austin/Chevron Bunionectomy - This is the most common bunion surgery performed for patients with a mild to moderate hallux valgus deformity. The goal of this procedure is to remove the bump and realign the joint. A “V” shaped cut is made at the head of the 1st metatarsal allowing the 1st metatarsal to shift laterally toward the second metatarsal bone. This bone cut will allow the bone to shift and the joint to realign. The bones are held together in this corrected position with screws. The screws are typically left in permanently unless they cause irritation of the soft tissues. The surgery is generally performed as an outpatient in a hospital or outpatient surgery center. Anesthesia is the choice of the surgeon made in consultation with the patient and anesthesiologist.
- Post-Operative Care
Patients have varying level of postoperative pain but quite often the pain is significantly less than what the patient anticipates. Following the procedure, the patient is immediately walking in a boot after surgery for 6 weeks or longer. Should the patient risk walking without a supportive shoe like the cam walker boot, they risk re-fracturing the bone and increase the duration of healing. The postoperative and rehabilitative course is improved by the use of ice and elevation of the extremity as much as possible. One of the most important aspects of the postoperative treatment is early motion of the joint to prevent joint stiffness. Once the bone has healed they can resume regular activity and begin wearing regular shoes.
Akin Bunionectomy - This procedure is used as an adjunct to other techniques such as the distal chevron osteotomy, proximal metatarsal osteotomies and the Lapidus procedure. The Akin osteotomy should not be used as the sole method of correcting a hallux valgus deformity. An angular cut is made at the big toe where a triangular wedge is removed. As a result, the wedge is closed down and the big toe is now in a straighter position. The bones are fixated with a screw so that the bone heals in the desired position.
Lapidus Bunionectomy - This procedure is used for a moderate to severe deformity and when there is a significant amount of hypermobility of the first ray. The entire 1st metatarsal is moved into a corrected position reducing the 1st and 2nd metatarsal angle while fusing into the cuneiform bone. The bones are fixated with screws and plate to allow for fusion. Once the bone heals and fusion is achieved, the screws are not needed and are generally not removed. With this type of procedure, the long bone can never move out of position. Patients are non-weightbearing in a cast for a minimum of 6 weeks.
- Possible Complications
Complications following bunion surgery are uncommon but may include infection, suture reaction, delayed or nonunion of the osteotomy, irritation from the screws, stiff joint or recurrence of the deformity. Recurrence of the deformity can be slowed with the use of functional foot orthotics. It is important to understand that surgery does not always correct the cause of the bunion deformity. Functional foot orthotics do address the cause of the deformity and their use is strongly encouraged following bunion surgery. A rare complication is the over correction of the bunion deformity.
